By Harlan M. Krumholz, M.D.*
 |
|
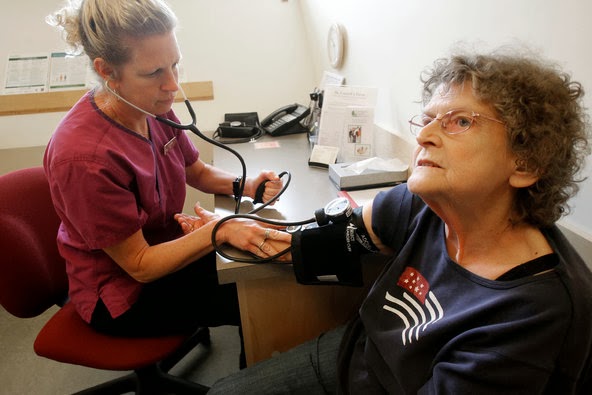
New guidelines suggest that people over age 60 can have a higher blood pressure than previously recommended before starting treatment to lower it. Toby Talbot/Associated Press
|
The long-awaited new hypertension guidelines will change how we approach patients with high blood pressure. Here are three things you should know about them.
First, the guidelines raise the systolic blood pressure (the top number of the blood pressure reading) threshold for drug treatment from 140 to 150 for people 60 and older.
You may be familiar with the idea that hypertension should be treated when your blood pressure is higher than 140/90 mm Hg. Now, based on studies, the experts suggest starting drug therapy only when the reading is 150/90 or higher. In fact, the authors, some of the most prominent experts in the diagnosis and treatment of high blood pressure, said that the goal of drug treatment is to lower the blood pressure below 150/90.
This recommendation immediately puts many people who had drug treatment started because of mild elevations in systolic hypertension in an overtreatment category. Many people currently on drug treatment would not have been recommended for treatment under these new guidelines, including those who had high-normal values and were being treated for so-called pre-hypertension, a condition never officially sanctioned for treatment.
Second, there is insufficient medical evidence to support a systolic blood pressure threshold for the drug treatment of people younger than 60.
Let me repeat that. After all these years of studying people with high blood pressure, the panel concluded that there was insufficient evidence to support a recommendation for this large segment of the population.
Now that did not stop the authors from expressing an opinion that we ought to stay with the current threshold of a blood pressure lower than 140 for those younger than 60. They argued that there was no reason to change what we have been doing – even though it has been based on opinion and not evidence. My take here is that the evidence for this threshold is weaker than most people might believe – and decisions about treatment need to acknowledge this uncertainty and defer to the preferences of patients.
The authors of the guidelines similarly also stated that we lack evidence for the right target for patients with kidney disease and diabetes. Given the lack of evidence, the authors settled on a recommendation of a goal of less than 140/90 for patients for people with kidney disease and also those with diabetes. This is a change for many people because many doctors have been seeking a systolic blood pressure goal of less than 130, but the authors noted that such a recommendation is not supported by any clinical trial.
Meanwhile, they do indicate that the diastolic blood pressure (the bottom number) should be less than 90, and for people age 30 and older there is evidence to support that recommendation.
Third, the guidelines recognize that the modification of a risk factor – in this case hypertension, which is a risk factor for heart attacks and strokes and premature death – by drug therapy does not necessarily mean that you have reduced someone’s risk for these adverse health events.
What we discovered in studies was that treating mild elevations of blood pressure with drugs does not reliably improve patients’ health. Although there is no question that drug treatment of very high blood pressure levels is beneficial, we now have several studies that failed to reduce risk by lowering blood pressure from mildly elevated to lower levels. Several studies sought to reduce risk by lowering blood pressure from mildly elevated to lower levels – and the surprising finding was that there was no benefit.
What this means is that drugs have many effects, and their effect on a single risk factor does not capture all they are doing and cannot convey their net effect on someone’s health. We have so many examples of trying to change risk factors with drugs and doing no good – or even harm – even as we make a single risk factor look better.
The authors of the guideline were influenced by these studies and did not default to the idea that more treatment is better. They reflected on what we know from studies that tested specific treatment strategies, which led them to be more conservative in their recommendations than previous guidelines.
Additionally, there are other important aspects of these guidelines. While they focus on drug treatment, they do emphasize the importance of a healthy diet, weight control and regular exercise. They make separate recommendations for black and white patients. They steer people away from beta-blockers for the treatment of high blood pressure. They steer black patients away from ACE inhibitors or angiotensin receptor blockers. They steer all people toward thiazide-type diuretics and calcium channel blockers.
In summary, this is a large paradigm change. The authors state that they did not intend to redefine what constitutes high blood pressure, but in effect they have now set it at 150/90 for the purpose of drug treatment of the general population. They have illuminated the weakness of our current body of evidence and made sensible recommendations given what we know.
The new guidelines are a reason for people being treated for high blood pressure to start 2014 with a discussion with their doctor, particularly if they started drug treatment for mildly elevated blood pressure.
As always, all decisions about your treatment should reflect your own preferences about whether the benefits are worth the risks. What these guidelines reveal is that many decisions about blood pressure treatment are being made with less evidence than we need. This is a call to action for studies that can equip patients facing decisions about treatment with the information they need.
*Harlan Krumholz is a cardiologist and the Harold H. Hines Jr. Professor of Medicine, director of the Yale-New Haven Hospital Center for Outcomes Research and Evaluation and director of the Robert Wood Johnson Clinical Scholars Program at Yale University School of Medicine.
Source: http://well.blogs.nytimes.com
Get more stuff like this
Subscribe to our mailing list and get interesting stuff and updates to your email inbox.